What is secondary cataract?
Secondary cataract, also known as posterior capsular opacification (PCO), is a common complication that can develop following cataract surgery. While cataract surgery removes the cloudy lens and replaces it with an artificial intraocular lens (IOL), the natural lens capsule remains intact to support the IOL. Over time, residual lens epithelial cells can proliferate and migrate to the posterior capsule, causing it to cloud and impair vision in the same way that the original cataract did.
Secondary cataracts can develop months or even years after the initial surgery, affecting roughly 20-50% of patients within five years of surgery. Secondary cataract symptoms include blurred vision, glare, light halos, and decreased visual acuity, all of which can have a significant impact on daily activities and quality of life.
A comprehensive eye examination by an ophthalmologist, who will use a slit lamp microscope to examine the posterior capsule for any signs of opacification, is usually required to diagnose secondary cataract. The condition is easily identifiable and distinct from other postoperative complications or primary cataracts.
The good news is that secondary cataracts are treatable, and medical advances have made this condition extremely manageable. Understanding the causes, symptoms, and treatment options is critical for patients who have had cataract surgery and are experiencing vision problems.
Secondary Cataract Care and Treatment
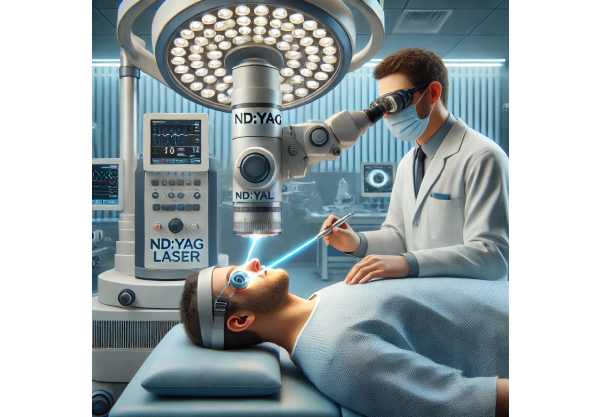
The primary treatment for secondary cataracts is a non-invasive, outpatient procedure known as Nd:YAG laser capsulotomy. This treatment is extremely effective and widely regarded as the gold standard for treating posterior capsular opacification.
- Nd:YAG Laser Capsulotomy: An ophthalmologist will perform a Nd:YAG laser capsulotomy, which is a simple and quick procedure. The patient’s pupil is dilatable with eye drops during the procedure. The ophthalmologist then uses a Nd:YAG laser to make a small opening in the cloudy posterior capsule. This allows light to pass through, restoring clear vision. The entire procedure usually takes only a few minutes and is relatively painless. Patients may experience floaters immediately following the procedure, but these usually disappear within a few days. Vision improvement is usually noticeable within a few hours to a day of treatment.
- Prevention Strategies: While Nd:YAG laser capsulotomy is effective, efforts are ongoing to reduce the incidence of secondary cataracts through preventive measures. Advances in IOL design, surgical techniques, and pharmacological interventions are being investigated to reduce the proliferation of lens epithelial cells after surgery. Some newer IOLs feature sharper edges, which can help prevent cell migration and lower the risk of posterior capsular opacification.
- Regular Monitoring: Patients who have had cataract surgery require regular follow-up visits with an ophthalmologist. These visits help to monitor for any signs of secondary cataract development and provide timely intervention if necessary. Early detection and treatment can help to prevent significant vision impairment while also maintaining quality of life.
- Patient Education: Educating patients about the possibility of secondary cataracts and the symptoms to look for is critical. Patients who are aware of their condition are more likely to seek immediate medical attention, resulting in earlier treatment and better outcomes.
Breakthrough Innovations in Secondary Cataract Treatment
The treatment landscape for secondary cataract has evolved significantly, with numerous innovative approaches and technologies transforming the management of this condition. These cutting-edge innovations aim to improve the efficacy, safety, and convenience of secondary cataract treatment, thereby improving patient outcomes and quality of life.
Advanced Laser Technologies
Nd:YAG laser capsulotomy remains the gold standard for secondary cataract treatment, but advances in laser technology are improving the procedure’s precision and safety.
- Femtosecond Laser-Assisted Capsulotomy: Femtosecond lasers, which are known for their accuracy and safety in cataract surgery, are being investigated for use in capsulotomy procedures. Femtosecond laser-assisted capsulotomy allows for more precise openings in the posterior capsule, potentially lowering the risk of complications and improving visual outcomes. This technology provides an alternative to the traditional Nd:YAG laser and may be especially useful in complex cases or patients with specific anatomical challenges.
- Improved Laser Delivery Systems: Advancements in laser delivery systems have improved the safety and efficiency of Nd:YAG laser capsulotomy. Newer systems include real-time imaging and automated tracking features, allowing ophthalmologists to perform the procedure with greater accuracy and less risk of causing accidental damage to surrounding ocular structures. These advancements ensure consistent and predictable results, which increases patient satisfaction.
Innovative intraocular lenses (IOLs)
Advances in IOL design are critical to preventing secondary cataracts and improving long-term visual outcomes following cataract surgery.
- Hydrophobic Acrylic IOLs: Studies have shown that hydrophobic acrylic IOLs reduce the incidence of posterior capsular opacification when compared to other materials. These lenses have a sharp posterior edge that prevents the migration of lens epithelial cells, lowering the risk of secondary cataract. According to studies, patients who have hydrophobic acrylic IOLs have a lower risk of PCO and may require fewer Nd:YAG laser treatments.
- Extended Depth of Focus (EDOF) IOLs: EDOF IOLs offer a continuous range of vision from close to intermediate distances, reducing the need for glasses while improving visual quality. These lenses are also intended to reduce the incidence of posterior capsular opacification. The combination of advanced optics and biocompatible materials in EDOF IOLs ensures better visual outcomes and reduces the risk of secondary cataract development.
- Preloaded IOL Delivery Systems: Preloaded IOL delivery systems make the implantation process easier and lower the risk of infection during surgery. These systems allow for more precise IOL placement, ensuring optimal positioning and lowering the risk of complications that could lead to secondary cataract formation. The use of preloaded systems also simplifies the surgical workflow, increasing efficiency and outcomes.
Pharmaceutical Interventions
Pharmacological intervention research is looking into new ways to prevent and treat secondary cataracts, potentially offering alternatives to laser procedures.
- Anti-Inflammatory Agents: Postoperative inflammation plays an important role in the development of secondary cataract. To manage inflammation following cataract surgery, anti-inflammatory agents such as corticosteroids and nonsteroidal anti-inflammatory drugs (NSAIDs) are common. Advances in drug delivery systems, such as sustained-release implants and topical formulations, are improving their efficacy in reducing inflammation and preventing PCO.
- Antiproliferative Agents: Antiproliferative agents are being studied for their ability to inhibit the growth and migration of lens epithelial cells. These agents can be administered during or following cataract surgery to prevent the formation of secondary cataracts. Research is being conducted to identify safe and effective compounds that can be incorporated into routine postoperative care to reduce the incidence of PCO.
- Gene Therapy: Gene therapy has the potential to prevent secondary cataracts by targeting the underlying cellular mechanisms that cause posterior capsular opacification. Experimental studies are looking into using gene editing techniques to change the expression of genes involved in cell proliferation and migration. While still in its early stages of development, gene therapy may provide a long-term solution for preventing secondary cataract.
Advanced Diagnostic Tools
Early detection and accurate assessment of secondary cataracts are critical for successful treatment. Innovations in diagnostic tools are improving ophthalmologists’ ability to diagnose and monitor PCO.
- OCT Imaging: Optical coherence tomography (OCT) generates high-resolution, cross-sectional images of the posterior capsule, allowing for a more detailed assessment of opacification and structural changes. Advances in OCT technology, such as swept-source OCT, provide deeper tissue penetration and faster image acquisition, increasing the accuracy and efficiency of secondary cataract detection.
- Scheimpflug Imaging: Scheimpflug imaging is a non-invasive technique for obtaining detailed images of the anterior and posterior segments of the eye. This technology is useful for determining the extent of posterior capsular opacification and developing an appropriate treatment plan. Scheimpflug imaging can also be used to assess the efficacy of interventions and identify early signs of recurrence.
- Artificial Intelligence (AI) and Machine Learning: AI and machine learning algorithms are being developed to analyze diagnostic images and predict the onset of secondary cataract. These technologies can help ophthalmologists identify patients at risk for PCO and optimize treatment plans. AI-powered diagnostic tools have the potential to enable more personalized and proactive management of secondary cataracts.
Patient Centered Care and Education
Advances in patient-centered care and education are improving secondary cataract management by providing patients with knowledge and support.
- Patient Education Programs: Comprehensive education programs assist patients in understanding the risks, symptoms, and treatment options for secondary cataracts. These programs are available in a variety of formats, including in-person consultations, online resources, and multimedia presentations. Patients who are educated are more likely to recognize symptoms early on and seek treatment as soon as possible, which improves outcomes and satisfaction.
- Telemedicine and Remote Monitoring: Telemedicine platforms allow for remote consultations and follow-up visits, providing patients with easy access to care. Remote monitoring tools, such as smartphone apps and wearables, enable patients to track their symptoms and communicate with their doctors. Telemedicine and remote monitoring improve continuity of care and ensure timely intervention for secondary cataract.
- Personalized Treatment Plans: Personalized treatment plans take into account each patient’s individual medical history, lifestyle, and visual needs. Ophthalmologists can improve outcomes and overall quality of life for those suffering from secondary cataracts by tailoring interventions to individual patients.