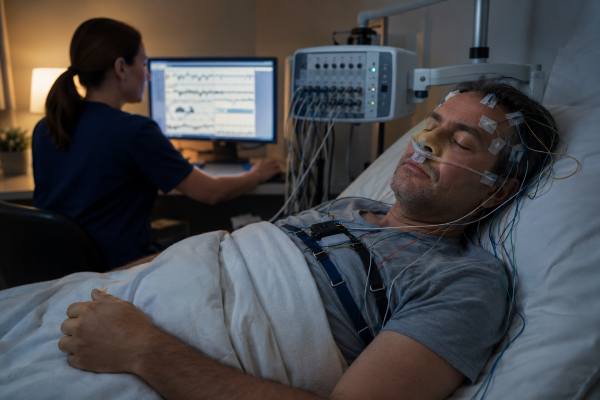
A sleep study can look simple from the outside: a night in a sleep lab, some sensors, and a report afterward. In practice, polysomnography is one of the most detailed ways clinicians measure what the brain, breathing, muscles, oxygen levels, and heart are doing during sleep.
The goal is not just to find out whether someone “slept badly.” A polysomnogram can show whether sleep is being disrupted by obstructive sleep apnea, central sleep apnea, limb movements, unusual behaviors during sleep, abnormal REM sleep muscle activity, low oxygen levels, or other patterns that may affect daytime fatigue, memory, concentration, mood, and safety. It does not diagnose every sleep or mental health condition by itself, but it can provide objective information that cannot be captured by symptoms alone.
Table of Contents
- What Polysomnography Measures
- When a Sleep Study Is Used
- Polysomnography vs Home Sleep Apnea Testing
- What Happens During the Study
- How Results Are Scored
- What Results Can and Cannot Tell You
- Next Steps After Polysomnography
What Polysomnography Measures
Polysomnography measures sleep as a whole-body process, not just as time spent in bed. A standard in-lab study records brain waves, eye movements, muscle tone, breathing, oxygen levels, heart rhythm, body position, and often audio or video so the sleep specialist can connect symptoms with objective events.
The “poly” in polysomnography matters. Sleep apnea, for example, is not diagnosed only by listening for snoring. Clinicians look at airflow, chest and belly effort, oxygen changes, arousals on brain-wave channels, sleep position, and sleep stage. This helps distinguish obstructive apnea, where breathing effort continues but airflow is blocked, from central apnea, where airflow and breathing effort drop together.
| Measurement | What it records | Why it matters |
|---|---|---|
| EEG | Brain-wave activity from scalp sensors | Identifies wakefulness, non-REM sleep stages, REM sleep, arousals, and sleep continuity |
| EOG | Eye movements | Helps identify REM sleep and transitions between sleep stages |
| Chin EMG | Muscle tone under the chin | Helps score REM sleep and detect abnormal muscle activity during REM |
| Leg EMG | Leg muscle activity | Detects periodic limb movements that may fragment sleep |
| Airflow sensors | Breathing through the nose and mouth | Identifies apneas, hypopneas, flow limitation, and breathing pauses |
| Chest and abdominal belts | Breathing effort | Helps distinguish obstructive, central, and mixed breathing events |
| Pulse oximetry | Blood oxygen saturation | Shows oxygen drops, oxygen burden, and recovery after events |
| ECG | Heart rhythm during sleep | Detects heart-rate changes and some rhythm irregularities during events |
| Position, audio, and video | Sleep posture, snoring, movements, and behaviors | Links events to back-sleeping, REM sleep, snoring, or unusual nighttime activity |
Some studies add carbon dioxide monitoring, especially when hypoventilation is suspected. This may be considered in certain lung, neuromuscular, obesity hypoventilation, or pediatric cases. During a positive airway pressure titration study, the recording may also include CPAP, bilevel PAP, or other pressure settings so the team can see which settings improve airflow, oxygen levels, and sleep stability.
A polysomnogram also measures sleep architecture: how long it takes to fall asleep, how much time is spent awake after sleep begins, how much sleep occurs in each stage, how often the person wakes briefly, and whether REM sleep appears at the expected time. These details are important because two people can both spend eight hours in bed but have very different sleep quality and physiology.
When a Sleep Study Is Used
A sleep study is used when symptoms or medical history suggest that something measurable during sleep may be disrupting breathing, movement, oxygen levels, alertness, or safety. It is most often ordered for suspected sleep apnea, but it can also help evaluate complex sleepiness, unusual movements, parasomnias, and certain sleep-related neurologic concerns.
Common reasons for polysomnography include loud habitual snoring, witnessed pauses in breathing, gasping or choking during sleep, morning headaches, high blood pressure that is hard to control, unexplained daytime sleepiness, or non-restorative sleep. People may also be referred when fatigue, poor concentration, or memory complaints do not improve with basic sleep habits. In that setting, a sleep study may be part of a broader evaluation rather than the only test needed.
Sleep disorders can overlap with cognitive and mental health symptoms. Untreated sleep apnea, chronic sleep fragmentation, restless legs, insufficient REM sleep, or circadian disruption can worsen attention, processing speed, emotional regulation, irritability, and depression-like fatigue. This is why clinicians may consider sleep testing when symptoms look like ADHD, depression, anxiety, or brain fog but sleep history raises concern. For a related discussion, see how sleep apnea can mimic ADHD, depression, and brain fog.
Polysomnography may also be ordered before a multiple sleep latency test, which is used to assess severe daytime sleepiness and conditions such as narcolepsy. The overnight study confirms whether the person had enough sleep and whether sleep apnea or another disorder could explain the daytime symptoms. The next-day test is a separate procedure, explained in more detail in MSLT sleep testing for excessive daytime sleepiness.
A sleep study is not routinely needed for every person with insomnia. Chronic insomnia is usually diagnosed through history, sleep patterns, and contributing factors. Testing becomes more useful when insomnia symptoms come with signs of sleep apnea, unusual behaviors, leg movements, neurologic concerns, or severe unexplained sleepiness. A clinical evaluation for chronic sleep problems can help determine whether a sleep study is likely to add useful information.
Urgent medical care is appropriate if nighttime symptoms occur with severe shortness of breath, chest pain, fainting, new confusion, seizure-like activity, sudden weakness, or other acute neurologic symptoms. Severe daytime sleepiness that makes driving unsafe also deserves prompt attention. A routine sleep lab appointment is not a substitute for emergency evaluation when symptoms suggest an immediate medical risk.
Polysomnography vs Home Sleep Apnea Testing
In-lab polysomnography is more comprehensive than most home sleep apnea tests because it measures actual sleep stages along with breathing and other body signals. Home sleep apnea testing can be useful for selected adults with a high likelihood of uncomplicated obstructive sleep apnea, but it is not designed to diagnose every sleep disorder.
A typical home sleep apnea test focuses on breathing: airflow, breathing effort, oxygen saturation, pulse rate, and sometimes position or snoring. Many home tests do not record EEG brain-wave data, so they estimate breathing events over recording time rather than confirmed sleep time. This can understate or distort severity in some people, especially if they lie awake for long periods.
In-lab polysomnography is generally preferred when the clinical picture is more complicated. Examples include suspected central sleep apnea, significant heart or lung disease, neuromuscular disease, opioid use, suspected hypoventilation, unexplained low oxygen levels, parasomnias, nocturnal seizures, REM sleep behavior disorder, severe insomnia that may interfere with home testing, or a previous home test that was negative or inconclusive despite strong symptoms.
The distinction matters because the question being asked determines the right test. If the question is “Does this otherwise uncomplicated adult likely have moderate to severe obstructive sleep apnea?” a home test may be reasonable. If the question is “What is happening to sleep stages, breathing effort, oxygen, movements, and behaviors across the night?” in-lab polysomnography is usually the more complete option.
Home testing also has a practical advantage: it is more familiar and may be easier to schedule. Some people sleep more naturally at home than in a lab. But convenience should not be confused with equivalence for all conditions. A home test that does not measure brain waves cannot fully describe sleep architecture, arousals, REM timing, or certain movement and behavior disorders.
A clinician may start with home sleep apnea testing when the situation fits, then recommend in-lab polysomnography if results do not match the symptoms. A common example is a person with loud snoring, witnessed pauses, and severe daytime sleepiness whose home test is technically limited or unexpectedly normal. In that case, the next step may be a full sleep study rather than assuming the symptoms are unrelated to sleep.
What Happens During the Study
A sleep study is usually painless, but it is more structured than a normal night at home. The main challenge is sleeping while sensors are attached; the equipment is designed to allow movement, bathroom breaks, and natural sleep positions as much as possible.
Before the test, the sleep center may ask about medications, caffeine, alcohol, usual bedtime, work schedule, medical conditions, and symptoms. Some people fill out sleepiness or sleep-quality questionnaires. One commonly used daytime sleepiness questionnaire is the Epworth Sleepiness Scale, which helps document how likely someone is to doze in everyday situations, but it does not replace objective testing when a sleep disorder is suspected.
On the night of the study, a technologist places sensors on the scalp, near the eyes, under the chin, on the legs, and on the chest. Belts go around the chest and abdomen to measure breathing effort. Small sensors measure airflow near the nose and mouth. A pulse oximeter is usually placed on a finger. Adhesive or paste is used to keep electrodes in place. The setup can take time, but none of the standard sensors should be painful.
Most sleep labs have a private room similar to a simple bedroom. The technologist monitors the signals from another room and can communicate through an intercom. If a sensor comes loose, the technologist may come in to fix it. If the person needs the bathroom, the technologist can disconnect or manage the equipment.
Some studies are diagnostic only. Others are split-night studies, where the first part of the night is used to diagnose sleep apnea and the second part is used to try positive airway pressure if enough events are seen early. In a full-night titration study, the main purpose is to adjust CPAP, bilevel PAP, or another treatment setting while monitoring breathing, oxygen levels, and sleep quality.
Preparation instructions vary, but common guidance includes washing hair without heavy oils or styling products, avoiding alcohol unless the clinician gives different instructions, limiting caffeine later in the day, bringing usual sleepwear, and taking regular medications only as directed. People should tell the sleep center about skin sensitivities, adhesive allergies, mobility needs, implanted devices, oxygen use, medications that affect sleep, and any safety concerns.
It is normal not to sleep perfectly in the lab. The first night in an unfamiliar place can reduce sleep time or change sleep stages. Clinicians account for this when interpreting the study. Even a shorter or somewhat restless night may still provide enough information, especially if it captures REM sleep, back-sleeping, oxygen changes, breathing events, or the symptom of concern.
How Results Are Scored
Polysomnography results are scored by reviewing the recording in short time segments and identifying sleep stages, arousals, breathing events, oxygen changes, movements, and rhythm patterns. The final report is not just a printout from a machine; it requires trained scoring and clinical interpretation.
Sleep staging is usually done in 30-second epochs. Each epoch is labeled as wake, N1, N2, N3, or REM sleep. N1 is light transitional sleep. N2 is a stable non-REM stage marked by features such as sleep spindles and K-complexes. N3 is deeper slow-wave sleep. REM sleep is associated with rapid eye movements, low chin muscle tone, and dreaming physiology. These stages help explain whether the person had enough consolidated sleep and whether certain events cluster in REM.
The report may include several sleep continuity measures:
- Sleep latency: how long it took to fall asleep.
- REM latency: how long it took to enter REM sleep.
- Total sleep time: how much sleep was recorded.
- Sleep efficiency: the percentage of time in bed spent asleep.
- Wake after sleep onset: how much wakefulness occurred after initially falling asleep.
- Arousal index: how often brief brain-wave awakenings occurred per hour of sleep.
For breathing, the most familiar number is the apnea-hypopnea index, or AHI. In adults, an AHI below 5 is often considered within the normal range, 5 to under 15 is commonly described as mild obstructive sleep apnea, 15 to under 30 as moderate, and 30 or higher as severe. These categories are helpful, but they do not tell the whole story. A person with “mild” AHI but major oxygen drops, severe sleepiness, high-risk work, cardiovascular disease, or events concentrated in REM sleep may still need careful treatment planning.
The report may also include oxygen desaturation index, lowest oxygen saturation, time spent below a certain oxygen level, snoring intensity, body-position effects, central apnea index, periodic limb movement index, and whether limb movements caused arousals. If REM sleep behavior disorder is suspected, the report may comment on REM sleep without normal muscle paralysis and whether video captured dream-enactment behavior.
Children are scored and interpreted differently from adults. AHI thresholds, oxygen concerns, symptoms, and treatment decisions are not identical across age groups. Pediatric sleep studies also require age-appropriate interpretation, especially when enlarged tonsils, growth, behavior, learning, or developmental concerns are part of the picture.
What Results Can and Cannot Tell You
A polysomnogram can show what happened physiologically during the recorded night, but it cannot explain every cause of fatigue, mood changes, poor concentration, or insomnia by itself. Its strength is objective sleep measurement; its limit is that sleep is only one part of a broader clinical picture.
A clear abnormal result can be highly useful. If the study shows obstructive sleep apnea with repeated oxygen drops and arousals, that may explain morning headaches, sleepiness, fragmented sleep, or concentration problems. If it shows frequent periodic limb movements with arousals, the next step may include checking for contributing factors such as iron deficiency, medication effects, or restless legs symptoms. If it shows abnormal REM muscle activity with dream enactment, a clinician may evaluate for REM sleep behavior disorder and related neurologic considerations.
A normal or near-normal study can also be useful, but it does not mean symptoms are imaginary or unimportant. Some problems vary from night to night. A single study may miss intermittent parasomnias, rare nocturnal seizures, or sleep apnea that occurs mainly with alcohol use, nasal congestion, REM sleep, or back-sleeping if those conditions were not captured. A person can also have severe sleepiness from insufficient sleep, circadian rhythm disorders, medication effects, depression, narcolepsy, idiopathic hypersomnia, chronic pain, or medical conditions that are not fully explained by the overnight recording.
Polysomnography is not a direct test for depression, anxiety, ADHD, dementia, or most psychiatric diagnoses. It can, however, identify sleep disorders that worsen or resemble those conditions. For example, someone with brain fog and poor concentration may need both sleep evaluation and broader medical or cognitive assessment. When symptoms are persistent or complicated, sleep studies for brain fog and fatigue may fit into a larger workup that also considers medications, mood, thyroid disease, anemia, B12 deficiency, pain, and sleep schedule.
The report should be interpreted in light of the person’s symptoms. AHI, sleep efficiency, REM latency, arousal index, and oxygen values matter most when connected to the clinical question. A technically adequate report that says “mild OSA” or “no significant OSA” may still require a follow-up conversation: Did the person sleep on their back? Was REM sleep captured? Were medications or alcohol involved? Were symptoms typical that night? Were there limb movements, arrhythmias, low oxygen levels, or unusual behaviors?
This is also why self-interpreting a sleep report can be misleading. The numbers are important, but they are not a complete diagnosis without context. A sleep specialist can explain whether the findings match symptoms and whether treatment, repeat testing, or evaluation for another cause makes sense.
Next Steps After Polysomnography
The next step after a sleep study depends on what the study found, how severe the findings were, and how well they explain the symptoms. Many people need a follow-up visit to review the report, discuss treatment options, and decide whether more testing is needed.
If the study shows obstructive sleep apnea, treatment may include positive airway pressure, oral appliance therapy, weight-related management when relevant, positional therapy, nasal or airway evaluation, or surgery in selected cases. CPAP is often recommended when apnea is moderate to severe, when symptoms are significant, or when oxygen drops and medical risks are concerning. Some people need a separate titration study, while others may start auto-adjusting positive airway pressure based on clinical judgment and insurance requirements.
If central sleep apnea, hypoventilation, or complex breathing patterns are found, follow-up may involve a sleep specialist, pulmonologist, cardiologist, neurologist, or medication review, depending on the pattern. These findings can require more individualized management than straightforward obstructive sleep apnea.
If the study suggests periodic limb movement disorder or restless legs syndrome, the clinician may ask about uncomfortable leg sensations, evening symptoms, medications, kidney disease, pregnancy, neuropathy, and iron status. In some cases, ferritin and iron testing are part of the follow-up. The sleep study can show the movements, but the diagnosis still depends on symptoms and clinical evaluation.
If abnormal nighttime behaviors are the concern, video findings may guide next steps. REM sleep behavior disorder, non-REM parasomnias, panic-like awakenings, and nocturnal seizures can look similar from a bed partner’s perspective but have different causes and treatments. Sometimes a standard PSG is enough; sometimes extended video EEG monitoring or neurologic evaluation is needed. A separate EEG test may be considered when seizure activity is part of the concern.
If results are normal, the follow-up should not stop at “nothing was found.” The clinician may review sleep schedule, circadian timing, medication effects, mood symptoms, pain, alcohol or cannabis use, caffeine timing, shift work, and medical causes of fatigue. When memory, confusion, or concentration problems persist, a broader evaluation such as brain fog testing may be appropriate.
The most useful question after receiving results is not only “Do I have sleep apnea?” but “Do these findings explain my symptoms, and what should change next?” A good follow-up visit should connect the data to a practical plan: treatment, safety precautions, repeat testing if needed, or evaluation for another cause.
References
- Australasian Sleep Association 2024 guidelines for sleep studies in adults 2024 (Guideline)
- Level 2 Polysomnography for the Diagnosis of Sleep Disorders: A Health Technology Assessment 2024 (Health Technology Assessment)
- Use of polysomnography and home sleep apnea tests for the longitudinal management of obstructive sleep apnea in adults: an American Academy of Sleep Medicine clinical guidance statement 2021 (Clinical Guidance Statement)
- Sleep Study 2023 (Review)
- Clinical Practice Guideline for Diagnostic Testing for Adult Obstructive Sleep Apnea: An American Academy of Sleep Medicine Clinical Practice Guideline 2017 (Guideline)
Disclaimer
This article is for general educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Sleep study results should be interpreted by a qualified clinician who can connect the findings with symptoms, medical history, medications, and safety concerns.
If you found this helpful, consider sharing it on Facebook, X, or your preferred platform so others can better understand what a sleep study actually measures.






