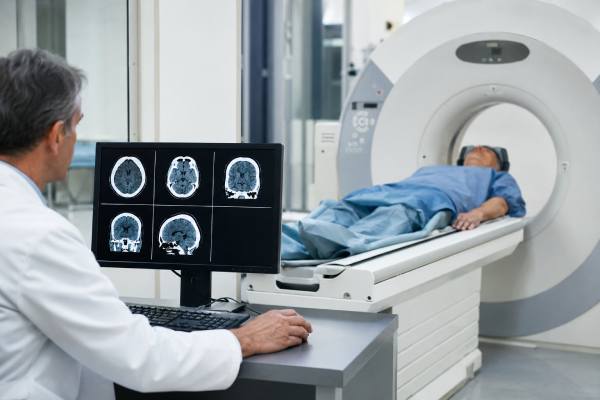
A brain CT scan is often used when doctors need a fast look at the brain, skull, and nearby structures. It is especially useful in emergencies, such as head injury, suspected bleeding in the brain, stroke symptoms, sudden severe headache, or a sudden change in alertness.
CT is not the most detailed test for every brain problem, and it does not replace a full neurological, cognitive, or mental health evaluation. Its main strength is speed: it can quickly show bleeding, swelling, skull fractures, some tumors, hydrocephalus, and other structural changes that may need urgent care. Understanding what CT can and cannot show helps make the results less confusing and helps people know what questions to ask next.
Table of Contents
- What a Brain CT Scan Shows
- When Doctors Order Brain CT
- What Brain CT Can Detect
- What Brain CT Cannot Show Well
- What Happens During the Scan
- Contrast, Radiation, and Safety
- Results and Next Steps
- When to Seek Urgent Care
What a Brain CT Scan Shows
A brain CT scan creates cross-sectional images of the head using x-rays and computer processing. It gives doctors a quick structural view of the brain, skull, blood spaces, ventricles, and some nearby tissues.
The word “CT” stands for computed tomography. During the scan, the machine takes many x-ray measurements from different angles and turns them into thin image “slices.” These slices can be reviewed one by one or reconstructed into different views. Compared with a regular skull x-ray, CT shows far more detail inside the head.
A standard head CT can show major structural problems, especially when there is a difference in density between tissues. Fresh blood, bone, air, cerebrospinal fluid, and many types of swelling or mass effect can often be seen clearly. This is why CT is so valuable when doctors need to know quickly whether there is bleeding, a fracture, pressure on the brain, or a large stroke.
Most emergency brain CT scans are done without contrast. “Without contrast” means no dye is injected into a vein. This is usually enough to look for acute bleeding, skull fractures, large areas of swelling, and many urgent problems after trauma. Some CT scans use iodinated contrast to make blood vessels, tumors, infection, inflammation, or abnormal enhancement easier to see.
A brain CT is different from a brain MRI. CT is usually faster and more available, and it is often the first test in emergency settings. MRI usually shows finer detail in brain tissue, especially for small strokes, demyelinating disease, subtle tumors, inflammation, and many chronic neurological conditions. The better test depends on the symptom, urgency, safety considerations, and what the doctor is trying to rule in or rule out.
CT is also different from cognitive or mental health testing. It can show some physical brain changes, but it cannot measure memory, attention, language, mood, anxiety, or executive function directly. For symptoms such as forgetfulness, poor concentration, personality change, or mood symptoms, CT may be only one part of a broader evaluation.
When Doctors Order Brain CT
Doctors usually order a brain CT when the information is needed quickly or when the symptom pattern raises concern for a structural brain problem. It is most often used for urgent symptoms, trauma, sudden neurological changes, or situations where MRI is not immediately available or not suitable.
Common reasons include head injury, especially when there is loss of consciousness, repeated vomiting, worsening headache, seizure, confusion, blood thinner use, older age, or signs of skull fracture. In these situations, CT can help identify bleeding, swelling, fracture, or pressure effects that may change treatment.
A CT scan may also be used when someone has symptoms of stroke, such as sudden weakness, facial drooping, trouble speaking, vision loss, severe dizziness with neurological signs, or sudden numbness on one side of the body. In suspected stroke, a noncontrast CT can help doctors look for bleeding, which is treated differently from an ischemic stroke caused by a blocked blood vessel. CT angiography or CT perfusion may be added in some stroke centers to assess blood vessels and blood flow.
Sudden severe headache is another important use. A “thunderclap” headache, especially one that reaches maximum intensity within seconds or minutes, may require urgent imaging to look for subarachnoid hemorrhage or other dangerous causes. CT may also be used when headache is accompanied by fever, cancer history, immune suppression, new neurological deficits, head trauma, pregnancy-related concerns, or a major change from a person’s usual pattern. For a broader comparison of imaging choices, MRI versus CT for brain symptoms can help clarify why one test may be chosen over the other.
Doctors may also order brain CT for a new seizure, sudden confusion, unexplained decreased alertness, suspected hydrocephalus, possible brain mass, complications of infection, or follow-up after certain neurosurgical procedures. In older adults, CT is sometimes used when new confusion, falls, or cognitive change raise concern for bleeding, a mass, enlarged ventricles, or other structural changes.
CT is not usually ordered just to “check the brain” for common mental health symptoms. Depression, anxiety, ADHD, autism, and many other psychiatric or neurodevelopmental conditions do not have a diagnostic CT pattern. Imaging may still be considered if there are red flags, such as new neurological signs, seizures, severe headaches, rapid cognitive decline, or a major change in consciousness.
What Brain CT Can Detect
A brain CT can detect many urgent structural problems, especially bleeding, skull fracture, swelling, hydrocephalus, and some large strokes or masses. Its strongest role is identifying conditions where fast treatment decisions matter.
| Finding or condition | How CT may help | Important limits |
|---|---|---|
| Bleeding in or around the brain | Can often show acute hemorrhage quickly, including subdural, epidural, intracerebral, and subarachnoid bleeding | Very small or older bleeds may need MRI or other follow-up testing |
| Skull fracture | Shows many fractures better than regular x-rays | Some facial, ear, or skull base injuries may need special CT views |
| Brain swelling or mass effect | Can show pressure, midline shift, compressed ventricles, or herniation signs | CT may not identify the exact cause without more imaging |
| Stroke | Can help distinguish bleeding from ischemic stroke and may show large established infarcts | Early ischemic stroke can be subtle or not visible at first |
| Hydrocephalus | Can show enlarged ventricles and pressure-related changes | Clinical context is needed to judge cause and significance |
| Brain tumor or mass | May show a mass, swelling, calcification, bleeding, or pressure effects | MRI is usually better for tumor detail and treatment planning |
| Sinus, skull, and some ear-region problems | May show sinus disease, bone changes, or trauma-related findings | A dedicated sinus, temporal bone, or facial CT may be needed |
Bleeding is one of the clearest and most important findings. After a head injury, CT can help detect an epidural hematoma, subdural hematoma, brain contusion, or bleeding inside the brain tissue. These findings can be life-threatening if they expand or increase pressure inside the skull.
CT is also useful for hydrocephalus, where the fluid-filled ventricles inside the brain become enlarged. This may occur from blocked cerebrospinal fluid flow, bleeding, infection, tumor, or other causes. In some older adults, enlarged ventricles may raise the possibility of normal pressure hydrocephalus, especially when walking difficulty, urinary symptoms, and cognitive changes occur together.
For stroke, CT is often used early because it is fast. A noncontrast CT can quickly show whether bleeding is present. If there is no bleeding and symptoms suggest ischemic stroke, doctors may use timing, examination findings, CT angiography, perfusion imaging, or MRI to guide treatment decisions. CT can also show some old strokes, brain tissue loss, and chronic small-vessel changes, although MRI is often more sensitive.
CT can detect some masses and tumors, particularly when they are large, calcified, bleeding, or causing swelling. However, a CT finding of a mass is often not the final answer. MRI with contrast is commonly used afterward because it provides more detail about the tumor’s location, borders, relationship to nearby structures, and possible causes.
In memory-loss workups, CT may be used to look for structural causes such as prior stroke, tumor, bleeding, hydrocephalus, or advanced brain atrophy. It does not diagnose Alzheimer’s disease by itself. More specific cognitive testing, lab work, MRI, PET imaging, or biomarker testing may be considered depending on the situation. For cognitive symptoms, brain imaging for memory loss is usually interpreted alongside the history and examination.
What Brain CT Cannot Show Well
A normal brain CT does not rule out every brain, cognitive, or mental health condition. CT is strong for many urgent structural findings, but it is less sensitive for subtle tissue changes, early ischemic stroke, many inflammatory disorders, and most psychiatric diagnoses.
Early ischemic stroke can be difficult to see on CT, especially in the first hours after symptoms begin. Doctors may still use CT first because it is fast and helps identify bleeding, but a normal early CT does not always mean there was no stroke. MRI with diffusion-weighted imaging is often better for detecting small or early ischemic strokes.
CT is also limited for many chronic or subtle brain disorders. Multiple sclerosis plaques, mild traumatic brain injury without bleeding, small tumors, low-grade inflammation, subtle infection, pituitary abnormalities, and many posterior fossa problems may be better evaluated with MRI. The posterior fossa includes the cerebellum and brainstem, where bone can interfere with CT detail.
A CT scan cannot directly diagnose concussion. A person can have a concussion with a normal CT because concussion usually affects brain function rather than causing visible bleeding or fracture. CT is used after head injury when doctors need to look for dangerous complications. Follow-up care may involve symptom monitoring, return-to-activity guidance, vestibular assessment, vision assessment, or concussion testing when symptoms persist.
CT also cannot diagnose depression, anxiety disorders, ADHD, autism, bipolar disorder, PTSD, or most other mental health conditions. These diagnoses are based on clinical evaluation, history, symptom patterns, functional impact, and sometimes standardized screening or neuropsychological testing. Brain imaging may be used when symptoms are unusual, sudden, severe, or accompanied by neurological signs. For this distinction, brain scans and mental health diagnoses should be understood as different kinds of assessment.
A normal CT result can be reassuring, but it does not mean symptoms are imagined or unimportant. Headache, dizziness, brain fog, memory problems, fatigue, mood changes, and concentration problems can come from many causes that do not show on CT. These include sleep disorders, medication effects, thyroid disease, vitamin deficiencies, migraine, anxiety, depression, infection, autoimmune disease, metabolic problems, and post-concussion syndromes.
This is why imaging is only one piece of the evaluation. The result must be matched to the person’s symptoms, timeline, examination, medical history, medications, and risk factors.
What Happens During the Scan
A brain CT is usually quick, painless, and noninvasive. The scan itself often takes only a few minutes, although registration, positioning, safety checks, and waiting for results can take longer.
Before the scan, a technologist may ask about symptoms, pregnancy possibility, allergies, kidney disease, diabetes medications, implanted devices, prior reactions to contrast, and recent imaging. For a noncontrast CT, little preparation is usually needed. People may be asked to remove glasses, hearing aids, hairpins, dentures, jewelry, or anything metal near the head that could affect the images.
During the scan, the person lies on a narrow table that moves through the CT scanner. The scanner is shaped like a large ring rather than a long enclosed tunnel. This makes CT easier for many people who feel claustrophobic in MRI machines. The technologist may use pillows or supports to keep the head still, because movement can blur the images.
The machine may make whirring or clicking sounds as it rotates. The technologist watches from a nearby control area and can communicate through an intercom. The scan is not painful, although lying still may be uncomfortable for people with neck pain, back pain, agitation, severe headache, or confusion.
If contrast is used, an IV line is placed, usually in the arm. Iodinated contrast can cause a warm sensation, a metallic taste, or a brief feeling of needing to urinate. These sensations usually pass quickly. The team will watch for allergic-like reactions, breathing symptoms, hives, dizziness, or other unusual symptoms.
Children and people who cannot stay still may need extra support. Many CT scanners are fast enough that sedation is not necessary, but sedation may sometimes be considered for young children or people who cannot safely complete the scan while awake. When children are scanned, imaging teams adjust the protocol to the child’s size and the clinical question.
After the scan, most people can return to usual activities unless the medical team says otherwise. If sedating medicine was used, driving and decision-making may be restricted for a period of time. If IV contrast was given, the team may advise drinking fluids unless there is a medical reason to limit fluid intake.
Contrast, Radiation, and Safety
Brain CT uses ionizing radiation, so it should be done when the expected medical benefit outweighs the risk. For many urgent symptoms, that benefit can be substantial because CT may identify bleeding, stroke, swelling, or injury that needs immediate treatment.
Radiation risk from a single medically necessary head CT is generally considered low, but risk is not zero. The risk is higher with repeated scans, multiphase studies, higher-dose protocols, and in children, who are more sensitive to radiation and have more years ahead for a radiation-related effect to develop. Imaging teams use dose-reduction strategies, especially in children, and doctors try to avoid CT when it is unlikely to change care.
Pregnancy is an important safety consideration. A head CT does not directly image the uterus, but anyone who may be pregnant should tell the doctor and technologist before the scan. In urgent situations, CT may still be appropriate. The decision depends on the medical risk of delaying diagnosis, the body area being scanned, and whether another test can answer the question safely.
Iodinated contrast is not used for every brain CT. It may be used when doctors need to assess blood vessels, infection, inflammation, tumor enhancement, or certain complications. It is commonly part of CT angiography, which looks at arteries or veins. Contrast can improve diagnostic detail, but it also adds considerations.
People should tell the medical team if they have:
- A prior reaction to iodinated contrast
- Kidney disease or reduced kidney function
- Diabetes medications, especially metformin, when relevant to local protocols
- Severe asthma or multiple allergies
- Thyroid disease
- Multiple myeloma or other serious medical conditions
- Pregnancy or breastfeeding concerns
Most contrast reactions are mild, such as itching, hives, warmth, nausea, or rash. Serious reactions are uncommon but can occur, so CT departments are prepared to treat them. Kidney-related precautions depend on the person’s kidney function, the urgency of the scan, the type and amount of contrast, and other risk factors.
Some people worry that CT will interfere with implants or devices. CT is generally less restricted than MRI for many implanted devices because it does not use a strong magnetic field. However, the imaging team still needs to know about implants, shunts, surgical clips, neurostimulators, hearing devices, and any recent procedures so the scan can be planned and interpreted correctly.
The safest approach is not to avoid CT categorically or request it automatically. The goal is appropriate imaging: using CT when it is likely to answer an important question, avoiding unnecessary scans, and choosing MRI, ultrasound, lab testing, observation, or specialist evaluation when those are better suited to the problem.
Results and Next Steps
Brain CT results are interpreted by a radiologist, then combined with the clinical picture by the treating clinician. The result may be normal, clearly abnormal, uncertain, or important but unrelated to the symptom that led to the scan.
In an emergency, a preliminary or urgent interpretation may be available quickly, especially if doctors are looking for bleeding, major stroke, mass effect, hydrocephalus, or fracture. A final written report may follow later. In non-emergency settings, results may take longer depending on the imaging center and ordering clinician.
A radiology report usually includes the exam type, reason for the scan, technique, findings, and impression. The “impression” section is often the most useful summary. It may say there is no acute intracranial abnormality, or it may describe bleeding, swelling, fracture, infarct, mass, enlarged ventricles, sinus disease, or age-related changes.
Some findings require immediate action. Examples include active bleeding, significant swelling, midline shift, hydrocephalus with pressure, large stroke, skull fracture with complications, or a mass causing pressure. These may lead to hospital admission, neurosurgery consultation, stroke treatment, repeat imaging, medication, or transfer to a specialist center.
Other findings require follow-up rather than emergency treatment. A CT may show an old stroke, chronic small-vessel ischemic changes, mild atrophy, sinus disease, calcifications, or an incidental cyst. These findings need context. Some are common with aging or vascular risk factors; others may need MRI or specialist review. A helpful next step is to ask the clinician which findings explain the symptoms, which are incidental, and what follow-up is recommended.
A normal CT can still lead to additional testing if symptoms continue or the clinical concern remains. Depending on the case, the next step may be MRI, CT angiography, lumbar puncture, EEG, blood tests, cognitive testing, sleep evaluation, medication review, or referral to neurology, neurosurgery, ophthalmology, psychiatry, or neuropsychology. For people recovering from brain injury, neuropsychological testing after concussion or brain injury may help assess attention, processing speed, memory, and executive function when symptoms persist.
When results are abnormal, it is reasonable to ask for a clear explanation in plain language. Important questions include: What did the scan find? Is it urgent? Does it explain the symptoms? Do I need MRI or another test? Should I avoid driving, work, sports, or certain medications? What symptoms should prompt emergency care? For broader follow-up planning, abnormal brain scan next steps can help frame the discussion.
When to Seek Urgent Care
A brain CT is often ordered after urgent symptoms, but the decision to seek emergency care should be based on symptoms, not on whether imaging has already been scheduled. Sudden neurological changes, severe head injury, or a rapidly worsening condition should be treated as time-sensitive.
Call emergency services or go to the emergency department for possible stroke symptoms, including sudden weakness or numbness on one side, facial drooping, trouble speaking, confusion, sudden vision loss, severe dizziness with trouble walking, or a sudden severe headache unlike usual headaches. Stroke treatment is time-dependent, and waiting to see whether symptoms pass can reduce treatment options.
Urgent evaluation is also important after head injury if there is loss of consciousness, repeated vomiting, worsening headache, seizure, unusual drowsiness, confusion, weakness, unequal pupils, fluid or blood from the ear or nose, suspected skull fracture, or worsening behavior changes. People taking blood thinners need a lower threshold for medical evaluation after head trauma, even when the injury seems minor.
Seek urgent care for a thunderclap headache, a new headache with fever and stiff neck, a headache with neurological symptoms, a new seizure, sudden severe confusion, fainting with injury, or a major change in alertness. In these situations, imaging may be only one part of the emergency workup.
Children, older adults, pregnant people, and people with cancer, immune suppression, bleeding disorders, recent brain surgery, or implanted shunts may need more cautious evaluation. Symptoms can be harder to interpret in these groups, and serious problems may not look typical at first.
Emergency evaluation does not always mean the CT will be abnormal. Many urgent CT scans are normal, and that can be useful information. The purpose is to identify or rule out dangerous problems quickly enough to guide care. For help recognizing when symptoms should not wait, ER-level neurological symptoms are best judged by suddenness, severity, and change from baseline.
References
- Head CT 2023
- Head injury: assessment and early management 2023 (Guideline)
- ACR Appropriateness Criteria® Head Trauma: 2021 Update 2021 (Guideline)
- ACR Appropriateness Criteria® Headache: 2022 Update 2023 (Guideline)
- ACR Appropriateness Criteria® Cerebrovascular Diseases-Stroke and Stroke-Related Conditions 2024 (Guideline)
- Manual on Contrast Media 2025 (Clinical Reference)
Disclaimer
This information is for general educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Brain CT decisions depend on symptoms, timing, medical history, examination findings, and safety factors, so discuss personal concerns and results with a qualified clinician.
Please share this article on Facebook, X, or your preferred platform to help others understand when brain CT scans are used and what their results can mean.






